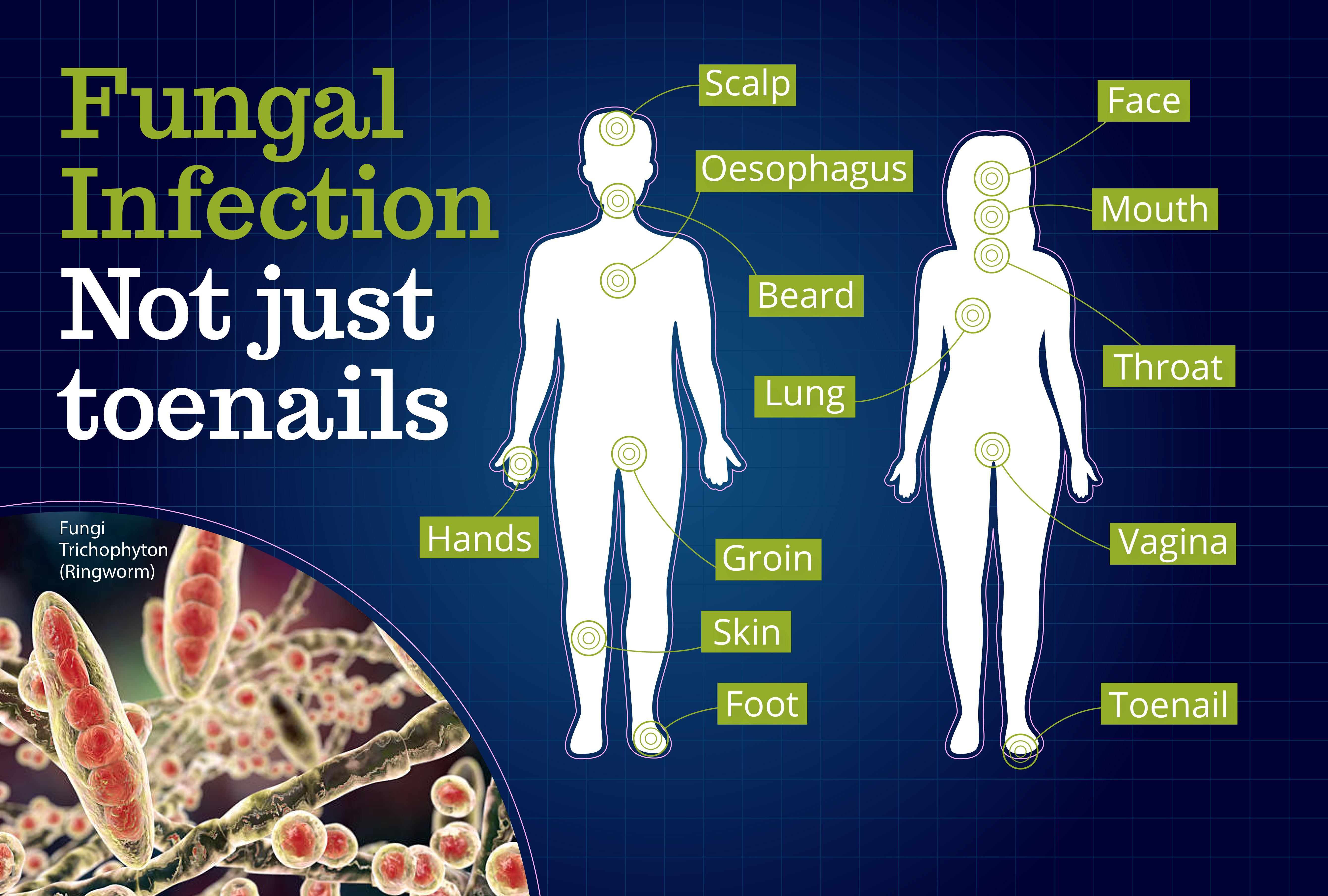
Onychomycosis (fungal nail infection) and tinea pedis (athlete’s foot), are some of the most common forms of fungal infection in adults and are often the first things that spring to mind when thinking of fungal infection. However, many other forms of fungal infection exist, which affect all different parts of the body and can have serious health implications.
Fungal infections are typically split into two types, Invasive Fungal Infections (IFIs) and Non-Invasive Fungal Infections, though it could be argued that all fungal infections are invasive due to their location within the body. IFIs, though rare, are typically systemic, severe and life-threatening,1, 2 while the more common non-invasive fungal infections are localised and generally benign.
Non-Invasive Fungal Infections
The most frequently occurring fungal diseases are the “non-invasive” infections such as fungal nail infection (tinea unguium), athlete’s foot (tinea pedis), ringworm (tinea corporis) and Candida infections of the vagina, mouth, throat, and oesophagus (Thrush).
The “tinea family” of infections are often caused by dermatophytes such as Trichophyton species, Epidermophyton species or Microsporum species and are named by site of infection. Tinea corporis (skin) and tinea capitis (hair) are more common in children. Adolescents and adults more often develop tinea cruris (groin), tinea pedis (athletes’ foot), and tinea unguium (nail). Fungal infection of the skin, hair or nails affects approximately 1 billion people worldwide 3 and, in the US alone accounted for 4 million outpatient medical visits.4
Almost everyone can get a tinea infection, but factors that increase risk include living in damp or humid areas, excessive sweating, participating in contact sport, wearing tight clothing and sharing clothing and linen.
Candidiasis (thrush) infections are usually caused by an overgrowth of Candida disrupting the normal balance of flora in the vagina or oropharynx. Repeated attacks of vulvovaginal candidiasis affect at least 135 million women a year worldwide with 5–10% of women having at least 4 attacks annually.5,6,7,8 The impact on quality of life is substantial.9 About 70% of all premenopausal women develop thrush at some point in their lives.10 This imbalance may be due to antibiotics, stress, and hormone imbalances, or poor eating habits, among other things. But notably oesophageal candidiasis is one of the most common infections in people living with HIV/AIDS with an estimated 2 million suffers worldwide.11,12,13
Non-invasive fungal infections are usually treatable with topical applications of anti–fungals, although for some indications, such treatments are only poorly effective. Systemic treatment may be required for persistent or more serious infections.
Invasive Fungal Infections
Invasive Fungal Infections are usually confined to those with weakened immune systems due to conditions such as HIV and some cancers, as well as immunosuppressive therapies associated with cancer and organ transplant. IFIs such as Candidaemia, infection with resistant Candida Auris, Candida peritonitis, Invasive aspergillosis (IA) and Pneumocystis pneumonia where fungal spores establish themselves within the internal organs pose a serious risk to health. These infections usually require aggressive and timely treatment with systemic, intravenous anti-fungal therapies, but often have extremely high mortality rates.
Approximately 400,000 Candidaemia cases are predicted worldwide, with a mortality of 30-55%.14 Candida peritonitis affects both those undergoing long term peritoneal dialysis for renal failure (CAPD) and post-surgical patients, usually in intensive care.
Over 300,000 patients develop IA annually with significant groups including those with acute leukaemia, transplant and COPD patients.14
Fungal (cryptococcal) meningitis, fungus spreading through blood to the spinal cord, and Pneumocystis pneumonia, a fungal infection of the lung by Pneumocystis jirovecii, pose a particular risk to those AIDs patients without access to antiretroviral therapy and as such are generally in decline in economically developed countries.15,16
Fungal disease can also be acquired from specific locations or as a result of allergy, injury or surgery. For example, valley fever fungus affects the lungs and is known to live in the soil in the southwestern United States and parts of Mexico and Central and South America.17 Additionally, fungal keratitis typically arises following surgery or injury to the eye, affecting 1 million to 6 million in SE Asia. Fungal keratitis is responsible for visual impairment in as many as 28.4 million people worldwide.18
4.8 million people with asthma develop Allergic Bronchopulmonary Aspergillosis (ABPA), a condition characterised by a hypersensitivity response to Aspergillus, while approximately 15% of people with cystic fibrosis develop ABPA.14 Severe Asthma with Fungal Sensitisation (SAFS), which is also caused by Aspergillus, though has a different clinical presentation, is predicted to affect ~6.5 million adults worldwide.14 Finally, allergic fungal sinusitis and rhinitis affects ~12 million people at any time.14
Overall, in healthy adults, non-invasive fungal infections are often easily treated and because of their “superficial” nature, may be easily dismissed as “trivial diseases”. However, they can have profound effects on the quality of life, especially if they become chronic in nature. More serious fungal infections can be highly problematic in older adults and young children, as well as other groups that have weaker immune systems. Timely, accurate diagnosis of infection is critical because, the sooner treatment is initiated for fungal infections, the better the outcome.
- P. Badiee, P. Kordbachev, A. Alborzi, S. Malekhoseini, M. Ramzi, H. Mirhendi, et al. Study on invasive fungal infections in immunocompromised patients to present a suitable early diagnostic procedure. Int J Infect Dis, 13 (2009), pp. 97-102
- B. De Pauw, T.J. Walsh, J.P. Donnelly, D.A. Stevens, J.E. Edwards, T. Calandra, et al. Revised definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer/Invasive Fungal Infections Cooperative Group and the National Institute of Allergy and Infectious Diseases Mycoses Study Group (EORTC/MSG) Consensus Group. Clin Infect Dis, 46 (2008), pp. 1813-1821
- Vos, T, Flaxman AD, NaghaviM et al, Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990—2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380:2163–96.
- Panackal AA, Halpern EF, Watson AJ. Cutaneous fungal infections in the United States: Analysis of the National Ambulatory Medical Care Survey (NAMCS) and National Hospital Ambulatory Medical Care Survey (NHAMCS), 1995-2004. Int J Dermatol 2009; 48:704-12
- Sobel JD. Vulvovaginal candidosis. Lancet. 2007; 369:1961-71.
- Foxman B, Marsh JV, Gillespie B, Sobel JD. Frequency and response to vaginal symptoms among white and African American women: results of a random digit dialing survey. J Womens Health 1998; 7:1167–74.
- Corsello S, Spinillo A, Osnengo G, Penna C, Guaschino S, Beltrame A, Blasi N, Festa A. An epidemiological survey of vulvovaginal candidiasis in Italy. Eur J Obstet Gynecol Reprod Biol 2003; 110:66-72.
- Foxman B, Muraglia R, Dietz, JP, Sobel JD, Wagner J. Prevalence of recurrent vulvovaginal candidiasis in 5 european countries and the United States: Results from an internet panel survey. J Low Genit Tract Dis 2013; 17:340-5
- Aballea S, Guelfucci F, Wagner J, Khemiri A, Dietz JP, Sobel JD, Toumi M. Subjective health status and health-related quality of life among women with recurrent vulvovaginal candidosis (RVVC) in Europe and the USA. Health Qual Life Outcomes 2013; 11:169
- Ferre J. Vaginal candidosis: epidemiological and etiological factors. Int J Gynaecol Obstet 2000; 71 Suppl 1:S21-7
- Buchacz K, Lau B, Jing Y, et al. Incidence of AIDS-Defining Opportunistic Infections in a Multicohort Analysis of HIV-infected Persons in the United States and Canada, 2000-2010. The Journal of infectious diseases 2016; 214:862-72
- Matee MI, Scheutz F, Moshy J. Occurrence of oral lesions in relation to clinical and immunological status among HIV-infected adult Tanzanians. Oral Dis 2000; 6:106-11.
- UNAIDS. Global HIV & AIDS statistics — 2018 fact sheet. Available from: http://www.unaids.org/en/resources/fact-sheet [Accessed 12/06/2019]
- Fungal Infection Trust. How Common are Fungal Diseases? Available from: https://www.fungalinfectiontrust.org/how-common-are-fungal-diseases [Accessed 12/06/2019]
- Harris JR, Balajee SA, Park BJ. Pneumocystis jirovecii pneumonia: current knowledge and outstanding public health issues. Curr Fung Infect Rep 2010;4:229-37.
- Centers for Disease Control and Prevention. C. neoformans Infection. Available from:https://www.cdc.gov/fungal/diseases/cryptococcosis-neoformans/index.html [Accessed 12/06/2019]
- Centers for Disease Control and Prevention. Valley Fever (Coccidioidomycosis). Available from:https://www.cdc.gov/fungal/diseases/coccidioidomycosis/index.html [Accessed 12/06/2019]
- World Health Organisation. Blindness and vision impairment. Available from: https://www.who.int/en/news-room/fact-sheets/detail/blindness-and-visual-impairment [Accessed 12/06/2019]